For US residents only
Understanding Pompe disease
When you’re managing Pompe disease, the value of information shouldn’t be underestimated. Learn what Pompe disease is, what causes it, and what symptoms it may lead to.
Ryan
Diagnosed with LOPD at age 31

Pompe disease at a glance
A rare, disease that can be classified into two subtypes:
Caused by in the acid alpha-glucosidase (GAA) gene, leading to a buildup of in the muscles
An inherited condition that can cause varying levels of disease severity, depending on how much GAA enzyme activity is present
What is Pompe disease?
Pompe disease is a rare, causing muscular weakness that eventually leads to impaired mobility and breathing problems. Pompe disease is also referred to as acid maltase deficiency and glycogen storage disease type II.
Pompe disease is caused by variations in the acid alpha-glucosidase (GAA) These variations lead to a deficiency in GAA protein, which limits the body’s ability to break down glycogen in the This buildup of glycogen damages the body’s muscles, affecting mobility. As the muscles that control breathing become affected, respiratory problems can begin.

In the United States, an estimated 1 out of every 28,000 babies are born with Pompe disease today.
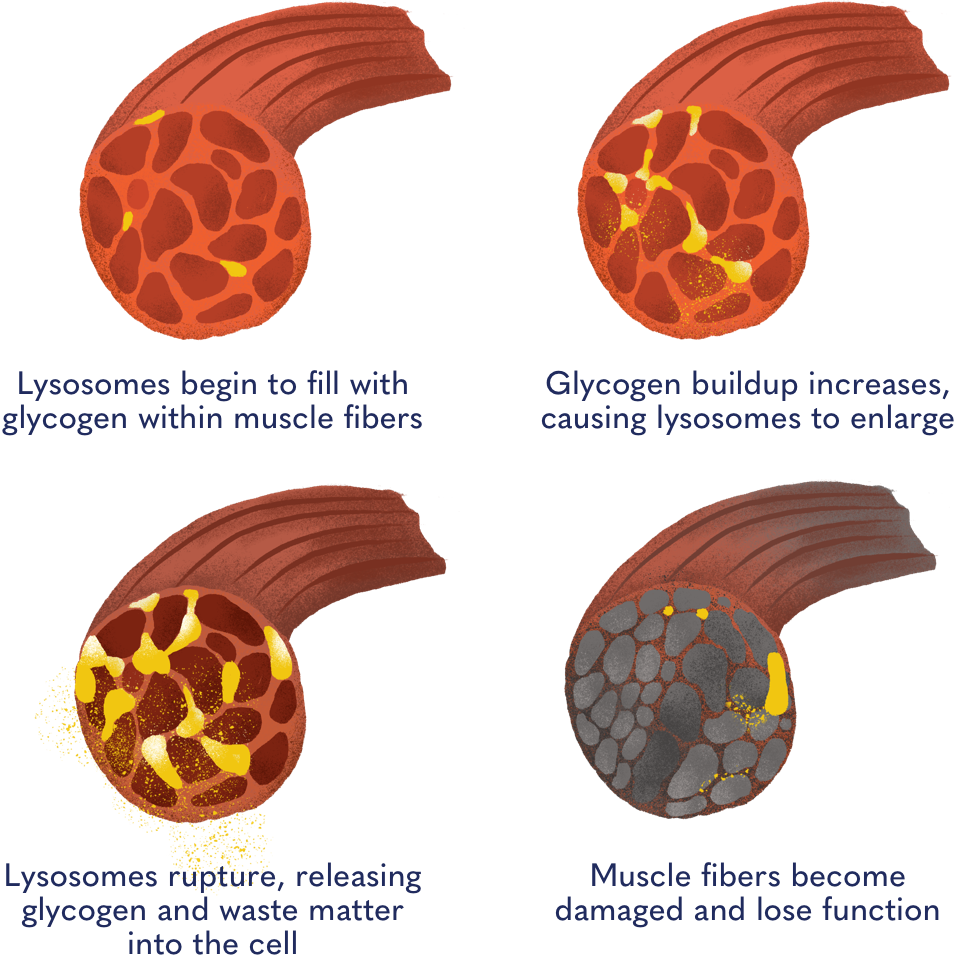
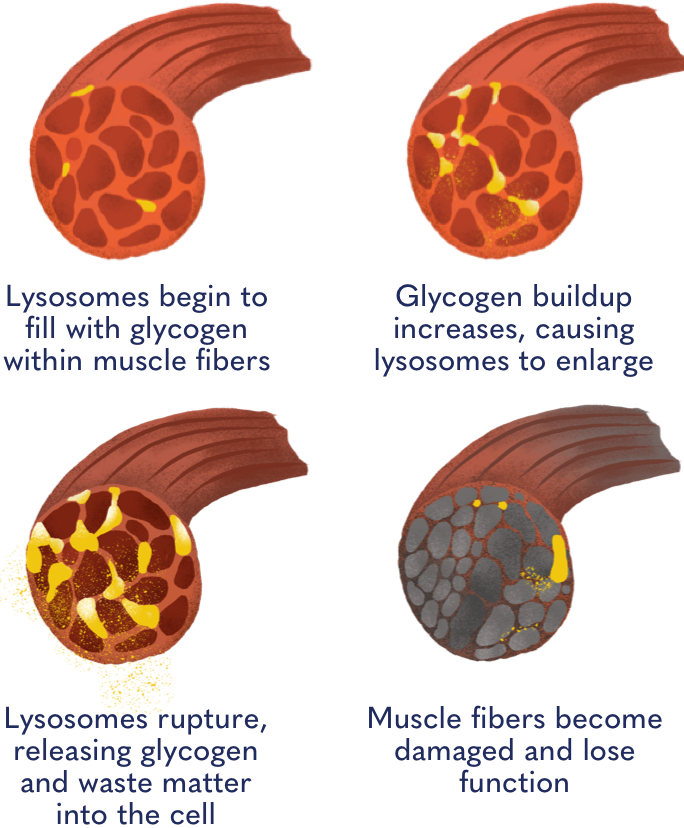
Glycogen: the real culprit
Although Pompe is caused by GAA gene glycogen is the real culprit. As steadily builds up in the of muscle tissue, it causes tissue and organ damage, and eventually leads to muscle deterioration. When the muscles that control breathing—such as the and the to deteriorate, respiratory problems may occur.
Because of this gradual loss of muscle control, many people with Pompe may eventually require assistive devices like canes, walkers, and wheelchairs over time. A ventilator may also be required to assist breathing, while any issues with swallowing or eating may eventually require the use of feeding tubes.
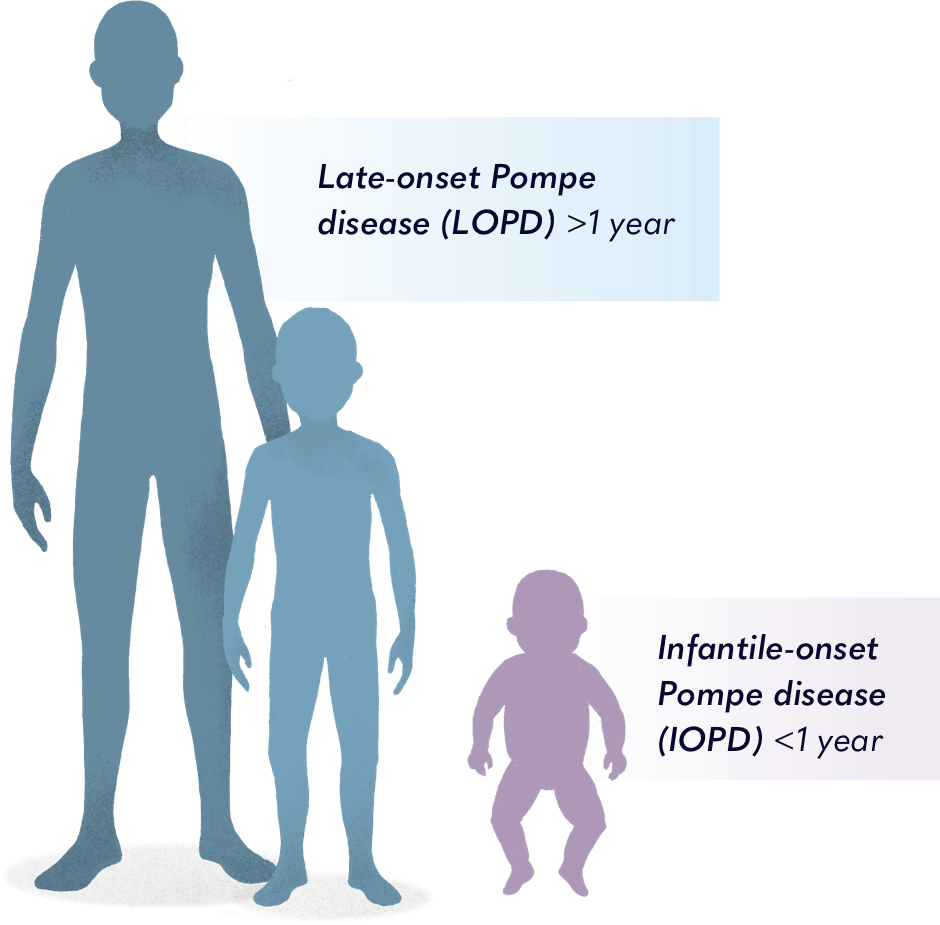
IOPD and LOPD
Pompe disease is classified into two subtypes: infantile-onset Pompe disease (IOPD) and late-onset Pompe disease (LOPD). In IOPD, symptoms typically appear during the first year of life and tend to progress very quickly.
With LOPD, symptoms may not be apparent right away, and can mimic those of other disorders. Symptoms of LOPD can present at any time, and most commonly consist of muscle weakness and breathing problems. But LOPD can also cause a range of other symptoms, including fatigue, digestive problems, difficulties with talking and chewing, and more. This can make LOPD very difficult to diagnose.
The importance of enzyme activity
People with IOPD have very low levels of GAA activity, with typically less than 1% of what’s considered normal. On the other hand, the levels of GAA enzyme activity can vary over a wide range (1% to 40% of what’s considered normal) in individuals with LOPD. That’s why no two people experience Pompe the same way.
What exactly does this mean? In terms of disease progression, it means a lot. The amount of GAA enzyme activity can impact how severe Pompe can become for each individual.
How is Pompe inherited?
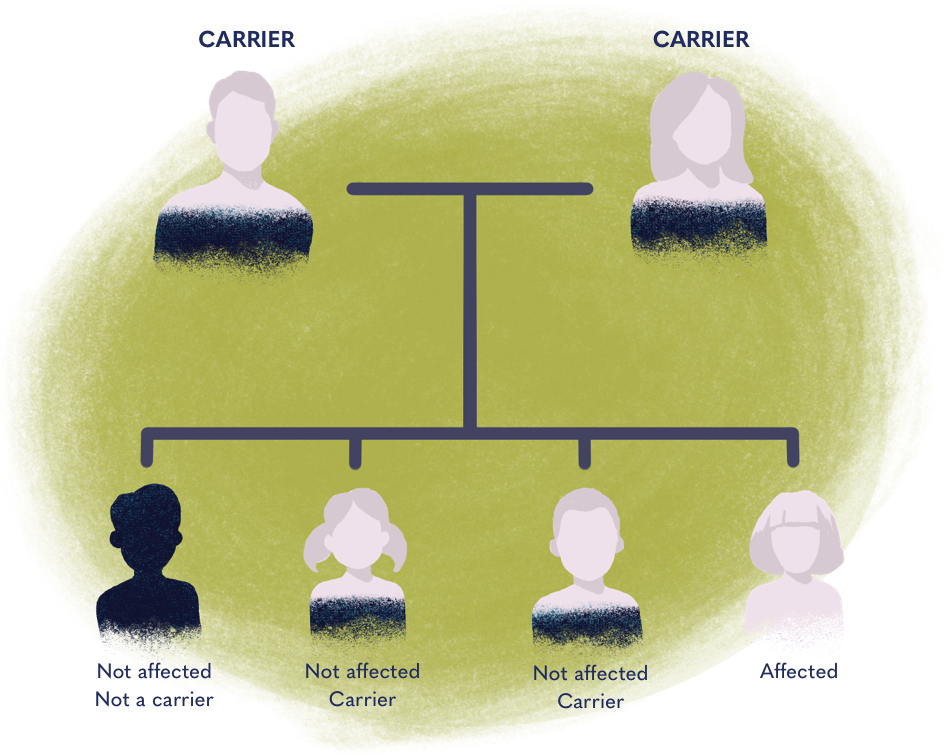
Every person inherits one copy of a gene from their father and one copy from their mother. Pompe is an disorder, meaning that a mutated version of the GAA must be inherited from both parents. If one of the two inherited GAA genes is normal, a person will not have Pompe disease, but would be considered a “carrier.”
Pompe disease carriers usually do not have any signs or symptoms of the disease. However, they can pass it down to their children. Whether or not a person develops Pompe disease depends on the genes they inherited from both their parents.
For in-depth information about how Pompe affects families, download the Pompe visual guide below.

Download the Pompe visual guide
Find easy-to-understand information about Pompe disease.

Early detection is everything
Pompe disease can be very difficult to diagnose. And while the presence of symptoms can help to establish a diagnosis, GAA enzyme and carrier identification screenings are required to confirm it. Newborn screening can lead to earlier detection and treatment, which is of utmost importance. Without proper treatment, most people with IOPD will succumb to the disease before the age of 1 year.
Your next chapter begins with you
When it comes to managing Pompe disease, there’s no one-size-fits-all approach. The best strategy for one person might not make sense for you, and vice versa. Individual choices should be made together with your healthcare team, and with both short-term and long-term goals in mind.
Stay Connected
Sign up to get the latest Pompe disease news and supportive information from Amicus Therapeutics.
What’s your pompe plan?
Discover ways to get proactive about your disease management.
